Hip & Groin Pain: exercise and sports related
Hip and groin injuries often affect football and rugby players as well as athletes taking part in running sports such as marathons and triathalons. The risks come from the repetitive fast changes in pace of running and a quick change of direction when twisting or pivoting in tackling.
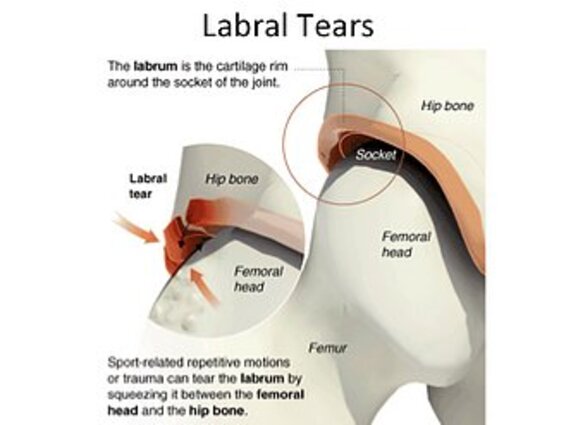
Labral Tear:
A labral tear occurs inside the hip joint and involves the labral cartilage layer. This is a flexible rubber-like lip at the edge of the socket of the hip. The hip is a ball and socket joint. The labral lip seals the joint for better fluid lubrication. A tear occurs because of a hard tackle or a kick when the joint is in a stressed position.
CAM Bony Bump:
The femoral head is normally round like a golf ball and this helps it to move freely within the socket. In some patients, the ball of the hip is not completely round but more egg shaped. This extra bony bump can jam up against the round socket causing a labral tear and pain. This is known as Femoro-Acetabular Impingement or CAM- FAI or Bump-FAI.
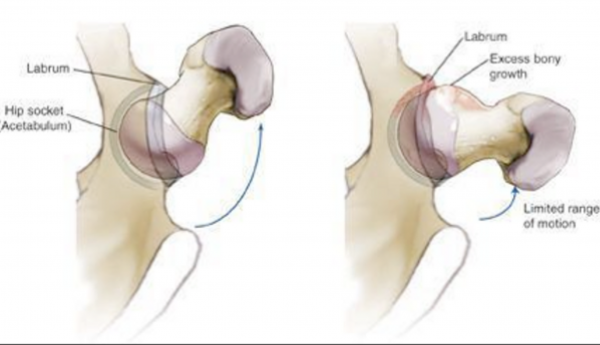
Pincer Lesion:
If the socket is not completely the correct shape or if its facing the wrong direction; facing too far backwards or downwards then a shelf of bone from the pelvis can hit the femur bone when the hip joint is moving. This typically happens when the joint is in a maximal position of flexion or extension and rotation. Typical for athletics, running, getting dressed or even just sitting into a car. This is called Pincer-FAI.
Gender differences: Females tend to have Pincer-FAI more, whilst males have CAM-FAI.
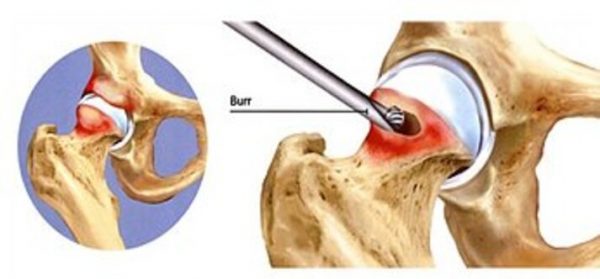
Picture showing the Pincer FAI or Extra Shelf of Bone overcovering the head on the left. The right shows a CAM or Bump FAI being shaved.
What are symptoms of FAI (Hip impingement)?
There is groin pain in the front skin crease and discomfort around the outer part of the hip and buttock area. It can feel like the hip is coming out of the socket and clicking in the hip can often be felt when moving the joint. Pain when putting on shoes or socks or getting in and out of a car is typical. Any movement that involves lifting the knee and twisting can make the pain worse.
What diagnostics are required? What technology is used?
A good clinical examination is always important. Plain x-rays are helpful but an MRI scan is the gold standard to show whether a labral tear has occurred. This will also detect if the ball has an extra bump of bone or whether the socket has any problems.
At Surrey Orthopaedic Clinic we have access to the latest technology that allows us to not only look at which parts of the body are injured, but also to check on the health status of the articular cartilage of that joint. This is a vital piece of information as it helps guidance in tailoring your individual treatment and options.
What treatment is required for FAI?
Rest and anti-inflammatories will alleviate the immediate pain. Activity modification and physiotherapy will also improve things further but if symptoms continue then an orthopaedic opinion will be required. An injection can help to get rid of the pain to allow rehabilitation, however if the problem comes back despite best efforts, an operation may be considered (Hip Arthroscopy) .
Hip Arthroscopy Surgery
What will Hip Arthroscopy surgery involve?
The operation will aim to repair the tear and remove the extra bony bump. This has good results in relief from the pain and will stop the ball and socket joint from jamming up preventing further damage to the joint cartilage.
What are the Risks of Hip Arthroscopy?
- Risks including infection and a fracture are about 1%.
- There may be an exacerbation of inflammation of the tendons and joint which may or may not need injections to these areas.
- Rarely, less than one in 200, the femoral or sciatic nerves or pubic area can get injured which usually are self resolving, may result in a foot drop and associated numbness.
- If there is arthritis, then the surgery is less likely to be successful and may come to a total hip replacement in due course.
- The tear and bump can recur but again, this is rare 1 in 200.
Depending on your medical fitness, there is a small chance of heart attack, stroke and risk of death 1 in 1000. If a fracture occurs in the hip then a hip replacement will need to be done as the chances of fixing the fracture and the head surviving without pain are low. The risk of this is 1 in 200.
We have made a joint decision for DVT and PE prophylaxes and we have decided to go ahead with bilateral TED stockings and Clexane injections for a fortnight to give mechanical and chemical thrombo-prophylaxes. Patients need to keep both feet mobile in order to activate the calf pump and keep the blood flowing through the legs to stop a clot forming as well as keep well hydrated.
The aim to reduce the level of the pain from 7-8/10 to 3/10 with a 80% success rate in addressing this aim.
Please have a look at the information that we will give you and consider things further and get back to us as necessary for any questions or to book your appointment.
How long will it take to recover from Hip arthroscopy?
Rehabilitation after surgery starts with 2 to 4 weeks protected weight bearing. Strengthening exercises take place at 6 to 8 weeks. Mean return to sport is 12 weeks.
There are three phases of rehabilitation the first phase using crutches to start to walk, phase two getting back onto normal mobility and phase three after three months getting back to more active lifestyle rehabilitation.
After surgery, you will have crutches for 4 to 6 weeks and be asked to put 10 to 30% of your weight onto the affected side for the first two weeks, then increase this to 30 to 50% in week 3 followed by 50% to full weightbearing from week 4 to 6. Physiotherapy will guide you through this using the protocol provided. Driving can only start after week 6 if your right leg is the one operated on or if you drive a manual car.
I advise you to use the painkillers regularly as it is easier to keep on top of the pain and exercise rather than be brave and suffer through this. I recommend regular paracetamol, codeine, pregabalin for two weeks and vitamin C and E for one month. We also give an antibiotic to reduce the chance of infection.
Surrey Orthopaedic Clinic Hip & Groin Pain Specialist:





