Rotator Cuff Tear of the Shoulder
ROTATOR CUFF TEAR
What is the Rotator Cuff?
The rotator cuff is made up of four muscles and their tendons that help move and stabilize the shoulder joint.
The four rotator cuff muscles include the:
- Supraspinatus
- Infraspinatus
- Teres minor
- Subscapularis
Rotator Cuff Tear
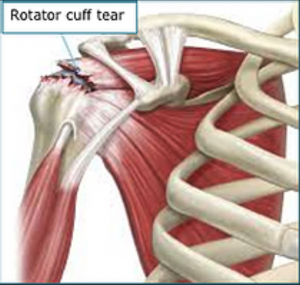
A Rotator cuff tear is a tear or detachment of the Rotator cuff tendon that attaches the muscle from the Scapula (Shoulder blade) to the head of the humerus.
Most tears occur in the Supraspinatus tendon.
Rotator cuff tears can be caused by injury i.e. traumatic cuff tears, repetitive stress, or bone spurs.
Note it is common for these tendons to tear as people get older i.e. degenerative cuff tears.
Tears can be full thickness or partial thickness.
Rotator cuff tears can cause pain and loss of function as well as weakness of the arm. The pain may cause difficulty in sleeping and difficulty in lifting objects away or overhead.
With time in the long term, chronic tears can cause increased pain and loss of function with disability. Tears do not generally heal by themselves. Chronic large tears may lead to arthritis
Diagnosis of Rotator Cuff Tears
At Surrey Orthopaedic Clinic our fellowship trained shoulder specialists doctors will examine your shoulder, assess the level of pain and limitations of how this is affecting you and perform diagnostic imaging – such as X-rays, Ultrasound and MRIs.
Your treatment will then be a tailored shared decision to suit your individual needs and aims. The physical, emotional and social aspects of your health will be discussed.
Treatment of Rotator Cuff Tears
Rest and anti-inflammatory painkillers will alleviate the immediate pain. Activity modification and physiotherapy to restore shoulder movement and strength, will also improve things further but if symptoms continue then an orthopaedic opinion will be required.
An injection can help to get rid of the pain to allow rehabilitation, however if the problem comes back despite best efforts, an operation may be considered.
Surgery may be considered early in large traumatic full thickness tears in younger patients.
Surgery – Arthroscopic Rotator Cuff Tear Repair
Arthroscopic (key-hole) rotator cuff surgery is performed using a combination of a local anaesthetic block and general anaesthesia. The local anaesthesia arm block is placed in the neck using ultrasound visualisation and numbs the affected shoulder and the arm for 12-24 hours.
Multiple small incisions (portals) are made around the shoulder to visualise and then repair the rotator cuff tendons. Sterile saline solution is pumped into and through the joint. This expands the shoulder joint to allow the surgeon access and space to visualise and perform the surgery.
Any spurs are removed on the acromium (Arthroscopic Subacromial decompression- ASAD).
The rotator cuff tear is then repaired. This involves stitching the torn tendon back to the bone using anchors. These are special screws (which become embedded into the bone) attached to a strong stitch (suture or tape) material which are placed through the torn rotator cuff tendons and then attached back to the humerus insertion site.
In order to make more space for the tendon repair, an arthroscopic subacromial decompression is performed at the same time. The technique usually requires 4-5 small (0.5cm) key- hole incisions.
Over 90% of the patients are satisfied at 18 months post-surgery, but it is not a “quick fix operation” and requires patience and hard work with adherence to a strict rehabilitation program supervised by your surgeon and physiotherapist.
Things you should know
- You can go home the day of surgery but usually stay overnight.
- The dressings are waterproof, so you can shower (out of the sling) resting your operated arm on your abdomen or by your side.
- Apply an ice pack regularly in the first few days after surgery to reduce pain and swelling.
- Take regular pain relief in the first few days, then as required.
- You will need to wear a sling full-time for 4-6 weeks (out of the sling to shower and dress).
- After 4-6 weeks – you can come out of the sling and start using the arm for usual gentle activities of daily living.
- Driving is NOT permitted until you come out of your sling.
- You will be advised when to start formal physiotherapy, usually at 4 to 6 weeks.
- The goal is to steadily achieve a normal range of shoulder motion, usually 3-6 months after surgery.
- Strengthening starts 3 months after surgery.
Risks & Complications (Arthroscopic Rotator Cuff Tear Repair Surgery)
All surgical procedures have the potential for complications.
The major potential problems during surgery include additional procedures to treat damaged structures, using bigger scars as well as bleeding or small nerve damage.
The major potential problems after surgery include stiffness and infection.
Infections can occur superficially at the incision or in the joint space of the shoulder, a more serious infection. Infection rates vary but are generally <1%.
Shoulder Stiffness is a common complication after all types of shoulder surgery. It is important to maximise pain management and comply with physiotherapy. If a post-operative frozen shoulder occurs it usually resolves by 9-12 months after surgery.
Despite the surgeon’s best efforts not all rotator cuff repairs will completely heal and may even retear.
Rare complications can occur from the local anaesthetic nerve blocks such as nerve damage.
Blood Clots (Deep Venous Thrombosis) can form in the arm or leg muscles and can travel to the lung (Pulmonary embolism). These can occasionally be serious and even life-threatening. If the patient suffers arm pain, redness or swelling, or have shortness of breath at any stage, contact the hospital immediately.
Serious medical problems can lead to ongoing health concerns, prolonged hospitalisation or rarely death. The risk of dying in the operating theatre under anaesthetic is extremely small. For a healthy person having planned surgery, around 1 person may die for every 100,000 general anaesthetics given.
As you might imagine, training and experience are very important in ensuring a good outcome for patients so we are delighted to say that we personally perform over 300 of these procedures per year including many revision cases for failed surgery from other centres as well as a large number of paediatric cases. We are recognised specialists in this operation and have pioneered new reconstruction techniques. This is reflected in both our results as well as our roles in training junior surgeons and fellow consultants in how to carry out these procedures.
Rehabilitation after Rotator Cuff Tear Repair
Rehabilitation aims:
- Achieve Range of Movement early
- Avoid stretching the repair for 6-8 weeks
- Strengthen the Rotator Cuff
- Hydrotherapy is beneficial
- Everyday use for daily activities is encouraged
- No antigravity exercise until 4 weeks
- No heavy lifting for 12 weeks
- Work – light duties from 6 weeks
0–3 Weeks:
- A Mastersling with a body belt and abduction pad attachment is worn for the first 3 weeks. The body belt is removed at 3 weeks leaving the sling only for weeks 3-6.
- Pain relief and ice as much as possible.
- Begin exercises including neck, elbow (active), wrist and hand range of motion with core stability work as necessary. Patient education and postural awareness with scapula setting; and relaxation of shoulder girdle.
- 3 Weeks: Consultant review and removal of abduction pad. Gentle pendular exercises (flexion, extension and circumduction).
4-6 weeks:
- Please consult the surgeon or operation notes. It is important to avoid forcing the repair and overstretching causing pain. The sling is gradually removed from 4-6 weeks
- If pain allows:
- Passive flexion (closed chain)
- Auto-assisted flexion (supine)- relax shoulder muscles sufficiently
- Supported passive ER
- Passive Abduction
- Begin hydrotherapy if available
- Begin active-assisted exercises
6–8 weeks:
- Start driving if comfortable
- Increase range of passive (6 weeks) movement then active (8 weeks) with functional movements at waist level, keeping arm close to body avoiding pain
- Closed chain exercises and proprioception
- Antigravity exercises may start once a good range of motion and shoulder control is obtained
8 weeks:
- Rotator cuff strengthening as pain allows
- Progress through active range of movement
- Correct abnormal movement patterns
12 weeks:
- Active arm elevation can start, initially while laying down, in water or with bent elbow (decreased lever arm).
- A rubber band strengthening program can commence with the upper arm and elbow remaining close by the chest.
6 months: resume full activities
What is Shoulder Impingement?
Shoulder Impingement or (Rotator Cuff Tendonitis) is when there is painful catching of the Rotator cuff tendon and the sac (above called the bursa) rub against a bony prominence of the shoulder blade known as the acromion.
This leads to inflammation and swelling of these structures and therefore further pinching. This pinching is worse every time the arm is raised so patients usually complain of pain when trying to lift the arm.
Over time, Shoulder Impingement can lead to inflammation of the bursa and damage to the rotator cuff tendons.
Symptoms of Shoulder Impingement
Pain:
- Radiating from the front of the shoulder to the side of the arm
- Pain with lifting and reaching out (painful arc)
- Pain at night
- Loss of strength
- Loss of range of motion
Shoulder Impingement is not life-threatening but can impact on a patient’s quality of life and function.
Shoulder Impingement can lead to inflammation of the bursa and rubbing on the rotator cuff. With time the rotator cuff tendons may degenerate further and tear.
Treatment of Shoulder Impingement
When discussing the most appropriate treatment for you our shoulder specialists will consider your individual circumstance and attitude including your age, activity level and general health.
Non-surgical Treatment
- Activity Modification: avoiding tasks that exacerbate the pain.
- Pain Management: Painkillers including Non-steroidal anti-inflammatory medication and cortisone injections
- Physiotherapy: to restore shoulder movement and strength.
Shoulder Impingement Surgery
Shoulder Impingement surgery is called arthroscopic subacromial decompression or ASAD and is performed as a keyhole (arthroscopic) minimally invasive procedure.
This requires either general and/or regional anaesthetic and is usually performed as a day case procedure.
It involves shaving part of the acromium to increase the space for the rotator cuff to reduce the chance of impinging or pinching.
A sling is provided for initial comfort and is removed as soon as pain allows (usually 2-3 days post surgery). Prior to discharge from hospital, you will see a physiotherapist who will give you a set of exercises to do. If your job does not involve raising your arm above the shoulder level or lifting, you should be back at work around one week after surgery. In the majority of patients, by 3 months symptoms should be 70-90% better compared to what they were before surgery however full improvement may take up to 9-12 months.
This procedure may also be performed with other procedures such as arthroscopic ACJ excision, arthroscopic rotator cuff repair and arthroscopic capsular release.
Arthroscopic Subacromial Decompression (ASAD) – Risks & Complications
Shoulder arthroscopy is a successful operation but like all operations there are some rare complications:
- Anaesthetic risks
- Recurrence of symptoms
- Incomplete resolution of symptoms
- Damage to nerve and blood vessels
- Stiffness
- Infection (risk less than 0.5%)
- Fracture (very rare)
- Chondrolysis (damage to the smooth articular cartilage surface lining of the shoulder joint surface – very rare).
- For ACJ excision: ACJ instability (if too much bone is shaved, then the collar bone can become unstable).
Serious medical problems can lead to ongoing health concerns, prolonged hospitalisation or rarely death. The risk of dying in the operating theatre under anaesthetic is extremely small. For a healthy person having planned surgery, around 1 person may die for every 100,000 general anaesthetics given. Arthroscopic Subacromial Decompression (ASAD)- Rehabilitation
Rehabilitation aims:
- Achieve full range of movement
- Active forward flexion and abduction to horizontal by 6 weeks, passive flexion, abduction and external rotation to normal by 6 weeks
- Strengthen the Rotator Cuff – If cuff deficient, introduce anterior deltoid strengthening exercises
- Improve postural awareness and initiate scapula stability
- Restore normal proprioception
- Slower progress with ACJ excision
It is important to avoid repetitive overhead activity at or above shoulder height for 3 months.
What is Calcific Tendinitis?
Calcific tendinosis is the abnormal deposition and build-up of calcium in the tendons of the rotator cuff muscles. The calcium can be very irritating to the local tendon causing extreme pain. The calcium can limit shoulder movement as it reduces the space between the rotator cuff and the acromion (the end of the shoulder blade), which can cause inflammation when the arm is raised.
Calcific tendinosis normally affects people in the age group of 30-50 years. Symptoms include intense pain on the outside of the shoulder that may affect sleep, cause stiffness and difficulty with overhead activities.
Calcific tendonitis usually disappears by itself but this can take up to 10 years.
Treatment of Calcific Tendinitis
When discussing the most appropriate treatment for you our shoulder specialists will consider your individual circumstance and attitude including your age, activity level and general health.
Non-surgical Treatment
- Activity Modification: avoiding tasks that exacerbate the pain.
- Pain Management: Painkillers including non-steroidal anti-inflammatory medication and cortisone injections.
- Physiotherapy: to restore shoulder movement and strength.
If your symptoms don’t improve you may be offered surgery to create more space between the rotator cuff tendons and acromion to reduce pain and increase the mobility of the joint. The procedure, which is usually done arthroscopically, also involves removing the calcium deposits.
The main risk of the surgery is stiffness (frozen shoulder) which eventually resolves but can cause significant symptoms. To avoid stiffness painkillers are prescribed and early range of motion exercises are commenced with a physiotherapist.
Other risks include infection, skin nerve injury and incomplete pain relief. Driving can begin 1-2 weeks after surgery.
Complete recovery can take 4-6 months.
Recurrence of the calcium lump in the shoulder is rare.
Surrey Orthopaedic Clinic Rotator Cuff Specialists:





